Transplant and Transition: How One Family Advocated to Get Their Choice Provider
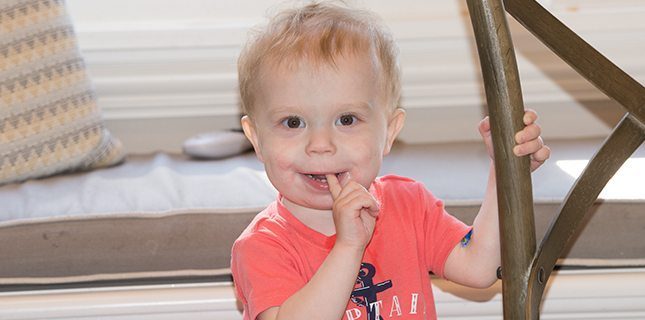
After doctors discovered an issue with her baby’s heart at 14 weeks gestation, Natalie had a closely monitored pregnancy and c-section at 39 weeks.
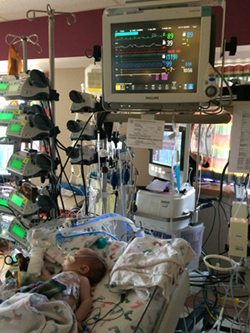
Her newborn son, Cameron, had a pacemaker placed shortly after birth, but doctors noticed his heart muscles were unusual – leading them to diagnose him with noncompaction cardiomyopathy. This congenital heart defect impacts the heart muscle’s ability to develop and pump correctly.
At just 28 days old, Cameron became the youngest heart transplant recipient at the Mayo Clinic and Natalie, along with her husband Robert and their older son, moved to Rochester for more than three months while their newborn recovered from this lifesaving procedure.
“Even once we came back, Cameron still had a lot of medical needs,” remembers Natalie. “Very frequent blood draws, feeding equipment and support were all crucial to ensuring our son was responding well to the transplant and getting the nutrients he needed to grow.”
Coming On Service With PHS
When Natalie and Robert needed nurses to do lab draws and patient assessments from their home, their insurance initially didn’t cover care from PHS and required they use a different home care provider. But after the first day with another nurse, Natalie knew they needed to negotiate to have care from PHS covered.
 “We eventually got approval, and have had Mary as our nurse for over a year and a half – and it’s been incredible,” said Natalie. “To bring two kids – one of who is in school and the other who is immunosuppressed – into a hospital or clinic for frequent tests just isn’t a viable option. This has been Cameron’s safest care option.”
“We eventually got approval, and have had Mary as our nurse for over a year and a half – and it’s been incredible,” said Natalie. “To bring two kids – one of who is in school and the other who is immunosuppressed – into a hospital or clinic for frequent tests just isn’t a viable option. This has been Cameron’s safest care option.”
With infusion nurse Mary’s weekly visits, Cameron is able to have vitals like blood pressure, weight, and height checked to ensure growth – crucial levels to track due to his history of feeding issues and transplant. She also does lab draws for what is needed from his following physicians and sends results to the Mayo Clinic – a process that encourages collaborative care that focuses on the best care plan for the family.
Natalie and her husband’s persistence to receive care from the the home care provider they wanted is something she says they knew was necessary for Cameron to get the best care. Through the utilization of many resources and a focus on advocating for their son, the entire family reaps the benefits of a strong personal and professional relationship with Mary and the infusion team.
Caring for the Whole Family
 When a child has medical complexities, it impacts the entire family. From schedules and school to sibling emotions, PHS recognizes the importance of ensuring a family can continue to live their life outside the demands of medical care. Cameron’s weekly lab draws fit into their family’s schedule seamlessly, and include his older brother – making the entire process less intimidating.
When a child has medical complexities, it impacts the entire family. From schedules and school to sibling emotions, PHS recognizes the importance of ensuring a family can continue to live their life outside the demands of medical care. Cameron’s weekly lab draws fit into their family’s schedule seamlessly, and include his older brother – making the entire process less intimidating.
“We’re a busy family – my husband and I both work, we have two kids, and his blood draws need to be done as a timed draw between 7:30-8:00am,” said Natalie. “Being able to receive Cameron’s care at home means we can still get his brother to school, and eliminate unnecessary exposure to illness. This way, both the boys are involved in the process – making it so much more relaxed and enjoyable for everyone.”
The Difference A Year Makes
When Natalie looks back at what her family’s life looked like this time last year, she realizes what incredible strides Cameron has made in his feeding and activity level.
 “Aside from his small size and medication needs, he’s just such a normal, happy, incredibly busy kid,” Natalie says. “People hear about him, but then are shocked when they meet him because he’s just a normal kid.”
“Aside from his small size and medication needs, he’s just such a normal, happy, incredibly busy kid,” Natalie says. “People hear about him, but then are shocked when they meet him because he’s just a normal kid.”
These days, Cameron loves to do everything older brother does, from climbing and dancing to trying to ride the big bikes and scooters. While eating has been a struggle throughout his entire life due to his prolonged intubation, he’s worked hard and now only uses his g-tube for medication purposes.
“He’s just a strong little boy in every aspect,” Natalie added.
Until Cameron no longer needs labs and assessments, PHS will be there helping this growing boy get stronger and stronger.


