Lila’s Story Part I: Over 13 Weeks of Bedrest and an Uncertain Future
We have a special treat in store for our readers over the next week. PHS mom, Aimee Tjader, has graciously offered to share her story. The story of her pregnancy, birth and coming home from the hospital with their new bundle of joy, Lila. Today, Aimee recalls the uncertainty she and her husband felt after an unexpected complication at only 18 weeks gestation. In the coming week we will be posting Aimee’s story in three parts. We will post part two tomorrow and the third the following Friday. Grab your box of tissues and read on as Aimee tells their story.
___________________________
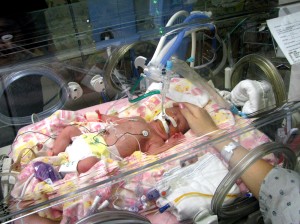
No parent can imagine their newborn baby hooked up to tubes and wires, fighting for their lives under a clear glass isolette in the neonatal intensive care unit (NICU). But for some families, the NICU is the best case scenario. It’s for those parents that the NICU is the “house of hope.”
At 18 weeks gestation, I suffered preterm Premature Rupture of Membranes (pPROM). In lamens terms, my water broke much too soon and the outlook was grim. Being my first pregnancy, I was clueless about such a condition. My heart sunk deep into my chest that day when the doctor confirmed I’d lost all of the amniotic fluid providing the protective pool around my baby. “What does this mean? Can’t something be done?”
Nothing could be done. I was told I would likely go into labor within a few days, or I could be admitted to the hospital right then and there to “take care of the situation” that night. I would have to deliver the baby, who obviously would not survive at 18 weeks. Or, in the slight chance that I stayed pregnant long enough the baby would likely have severely underdeveloped lungs (baby’s drink amniotic fluid to grow their lungs), deformities and other lifelong problems.
Trying to soak in this whirlwind of new information, I asked to be admitted for a round of IV antibiotics to ward off any potential infection brewing and for a Level III ultrasound by a high-risk doctor the next morning. I hoped and prayed that night, my first-ever night spent in a hospital, that the amniotic sac would heal and everything would be OK. In my dreams I would leave the hospital, still carrying my child, and get back to life as I knew it before I learned what pPROM was. I envisioned going back to work, growing a big round belly, having a baby shower and perusing the baby section of Target along with all the pregnant women. I’d stand proudly beside my pregnant best friend comparing our bellies for a photo op. And I’d create the perfect nursery with the baby’s name in giant script above the crib. But I never got to do any of that.
After one day in the hospital, I went home and under the advice of my doctors, got into bed and stayed there. We had a plan: I would complete six weeks of strict bedrest at home and once I reached 24 weeks gestation — viability — I would be admitted to the hospital until I delivered the baby.
The days dragged on. And on. Of course I was filled with fear that I would go into labor and everything would come crashing down in an instant, but I laid still in bed only getting up to use the bathroom and take quick showers. Friends, family and co-workers brought groceries and prepared meals, walked the dogs and cleaned the house. The support around us was incredible — it felt like all of Minnesota and every corner of the U.S. was pulling for our happy ending.
At 24 weeks, incredibly still pregnant, I was admitted to the hospital. With every intention of being there for the long haul, I brought the comforts of home: my own bedding, a rug, pictures, even a bedside lamp for cozy reading. I quickly got to know all of the antepartum nurses and all of the perinatologists. I sensed the sorrow in their voices and read the pessimism on their faces when I asked them about my outlook and the chance for a healthy baby. Every day they would check on me growing increasingly surprised that I was still there, my belly getting bigger with each week. I was hooked up to the fetal heart rate monitor twice-a-day and I received weekly ultrasounds, always showing a disappointing “unmeasurable” amount of amniotic fluid.
But I never gave up hope. I took vitamins, drank enough water to fill Lake Superior in hopes of creating more amniotic fluid, and did acupuncture, guided imagery and breathing techniques to keep me in a place of calm so that I could be the healthiest vessel for my baby. I was allowed to go for one wheel-chair ride a day outside, which I often took advantage of to savor Minnesota’s warm summer sun.
After celebrating making it to 31 weeks of pregnancy and seven weeks of hospital bedrest, I began to have contractions. They grew closer together, the baby had an elevated heart rate and I had a fever. The doctor called, feared an infection and said it was time. We would be having a baby that night and she would be here nine weeks too early.
 A quick ultrasound revealed the baby still in breech position, so I signed some papers and was wheeled off to the operating room. The room was bright, like in a dream, and freezing cold. My teeth chattered as they inserted the spinal and draped a blue cloth over my belly. A dozen doctors and nurses were on hand for the delivery, plus another handful waiting for our baby in the next room, including neonatologists and respiratory therapists. It was a scene straight out of some thrilling medical TV drama.
A quick ultrasound revealed the baby still in breech position, so I signed some papers and was wheeled off to the operating room. The room was bright, like in a dream, and freezing cold. My teeth chattered as they inserted the spinal and draped a blue cloth over my belly. A dozen doctors and nurses were on hand for the delivery, plus another handful waiting for our baby in the next room, including neonatologists and respiratory therapists. It was a scene straight out of some thrilling medical TV drama.
At 3:59 a.m. on Sept. 14, 2010, Lila Kalét Tjader arrived weighing 3 lbs. 14 oz. She didn’t cry, but she was beautiful. Tears welled up in my eyes as she was taken out of my sight. I crossed my fingers and repeated under my breath, over and over, “Breathe, baby, breathe.”
Originally published: December 29, 2011



My name is Roxana. My story is very similar to yours, but in my case my water broke at 13 weeks of gestation. We learned the news during a level 2 ultrasound at 18 weeks of gestation. The doctors adviced termination but I declined twice. i told them that We believe in God and that everything is in His mighty hands, and in His perfect wisdom and will. I managed to stay pregnant, I stayed in bed rest and at week 23 was admitted to the Hospital to continue the bed rest. I had ultrasounds once a month, I had as many people as I encountered, and family and friends praying for her,and at week 29 and 3 days my daughter Grace Miryam was born. She needed help with breathing. She is 1 month old, 4 lbs and 1 oz. She has met all her developmental milestones and is a healthy girl. Though she is still in NICU, she is doing wonderfully. She stil needs to learn to bottle feed, and to breathe on her own. Doctors stil amazed of her strength. We will bring her home soon! Some of the doctors have learned that God Allmighty is sovereign of all life. There is nothing impossible for God!
I niece also encountered this kind of unbearable case. We were so sad and nervous whenever he enters the operating room. We were always praying and kneeling to God to give him a chance and witness this wonderful world. Unfortunately, he died and our world became pale and unactive. It seemed that we lost our joy and and dreams.
I’m so sorry for your loss. You now have an angel in heaven looking over you. Our thoughts are with your family and we wish you the very best.
Roxana, what a fantastic story! Your family truly is blessed with your own little miracle baby. Congratulations on all of the milestones you have met and for your courage to keep your faith and stay strong throughout your pregnancy. From everyone here at PHS we wish you all the very best.