Thriving at Home, Thanks to Parenteral Nutrition
To round out HPN Awareness Week, we want to highlight PHS kiddos who are living at home, with their families, thanks to dietitians, infusion nurses and pharmacists nearby. Parenteral nutrition provides nutrients for individuals who cannot receive them through oral feeding, and in some cases can be the sole method of nutrients.
Our clinicians provide seamless, comprehensive care to ensure each kiddo they care for stays happy and healthy, and we are happy to see when families are able to enjoy those benefits too. Check out what Elias’ and Emma’s moms had to say about receiving parenteral nutrition at home, and then read on to hear from their PHS dietitians.
Do you use home parenteral nutrition? Share your stories in the comments!
A Focus on Elias’ Needs
His mom on receiving parenteral nutrition at home
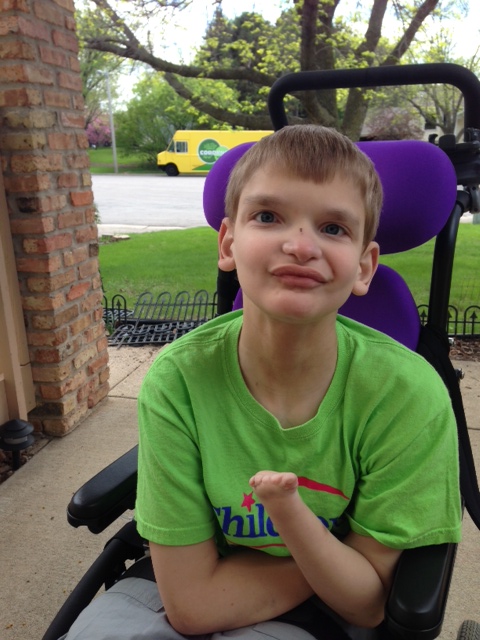 Elias receiving this service at home means we can be with him and participate in fine tuning his nutritional needs for recovery and growth, which enables him to have a better quality of life. Without the parenteral nutrition provided at home by PHS, my son wouldn’t probably be thriving as he is. The dietitians we have had throughout the years have helped keep our son from declining more and even in some cases implemented ideas with our doctors that have literally saved him from nutritional failure.
Elias receiving this service at home means we can be with him and participate in fine tuning his nutritional needs for recovery and growth, which enables him to have a better quality of life. Without the parenteral nutrition provided at home by PHS, my son wouldn’t probably be thriving as he is. The dietitians we have had throughout the years have helped keep our son from declining more and even in some cases implemented ideas with our doctors that have literally saved him from nutritional failure.
Parenteral nutrition allows our son to be able to live, play, and grow at home where chances of survival are greater. This is the true meaning of thriving at home.
Maria Mahady, PHS Registered Dietitian Supervisor, on being able to take care of kiddos like Elias at home
 My favorite part of developing plans for HPN patients is to watch their progress as they work towards and meet nutrition goals. When calculating nutrition plans for each HPN patient, their specific needs based on medical status tolerance levels, daily life schedules, etc. are taken into consideration. This involves really getting to know not only the patient, but the family involved in their care. Based on this patient and family-specific information, a plan is designed that allows them to thrive nutritionally while still allowing them to be a child with their family and have the life they deserve.
My favorite part of developing plans for HPN patients is to watch their progress as they work towards and meet nutrition goals. When calculating nutrition plans for each HPN patient, their specific needs based on medical status tolerance levels, daily life schedules, etc. are taken into consideration. This involves really getting to know not only the patient, but the family involved in their care. Based on this patient and family-specific information, a plan is designed that allows them to thrive nutritionally while still allowing them to be a child with their family and have the life they deserve.
At PHS, we have a multidisciplinary team that reviews each patient every 1 – 2 weeks to make sure we have researched every possible avenue to make advancements toward nutrition goals. This clinical team includes infusion nurses, dietitians, and pharmacists. Every individual that is a part of this team brings a different perspective and new ideas that further the quality of care our patients receive.
One home visit to see Elias that I will never forget is the time his PHS infusion nurse and I were walking up the driveway and looked up to see him standing up at the window waving. He had a big smile on his face… it melted my heart and absolutely made my day!
Emma Stays Healthy at Home
Her mom on being able to enjoy life, thanks to HPN
 Emma has been G-tube (or G/J-tube) fed since February 2008 (when she was 10 months old) and has been on TPN, besides a short break last year, since January 2010.Sometimes Emma has been able to have oral feedings if her stomach is working well enough for her to have them, but it also depends on what her respiratory status is – if she’s having respiratory issues, then she can’t have oral feedings due to her history of silent aspiration.
Emma has been G-tube (or G/J-tube) fed since February 2008 (when she was 10 months old) and has been on TPN, besides a short break last year, since January 2010.Sometimes Emma has been able to have oral feedings if her stomach is working well enough for her to have them, but it also depends on what her respiratory status is – if she’s having respiratory issues, then she can’t have oral feedings due to her history of silent aspiration.
Emma has used or is currently using PHS infusion nursing & pharmacy, dietitians, receives supplies, and also has used the respiratory team. Having the services in the home is a great help because otherwise Emma would be in the hospital and when she’s there, she is more likely to come home with another type of illness. Thanks to parenteral nutrition at home, Emma is able to go to school and make friends (and enjoy life). We’re also able to take her to family functions and she’s able to be a “normal” kid… or Emma’s normal.
Rachael Halvorson, PHS Clinical Dietitian, on adapting care to each kiddo’s lifestyle
 My favorite part of developing plans for HPN patients is the ability to create a plan that fits in with the family and patient’s life. If the kiddo is set to go to school and we want to have the HPN off during this time, I can adjust the HPN to accommodate for it. This allows kids who receive HPN to have as normal of a life as possible while still receiving life sustaining therapy.
My favorite part of developing plans for HPN patients is the ability to create a plan that fits in with the family and patient’s life. If the kiddo is set to go to school and we want to have the HPN off during this time, I can adjust the HPN to accommodate for it. This allows kids who receive HPN to have as normal of a life as possible while still receiving life sustaining therapy.
I have also had a few cases where I saw a child transition from parenteral to oral nutrition, and it is extremely rewarding to help families facilitate meeting their calorie needs from food rather than having to be hooked up to infusion therapy. However, the ability to transition is often dependent on the specific medical condition and why they were started on HPN.
The last time I was out to the home to visit Emma, her dad had Emma in his lap and was playing with her and Emma was full of belly laughs and giggles. It was such a wonderful moment to be able to see how well Emma has done in the home with the help of her PHS family. During these home nutrition visits, I typically identify what the family schedule looks like in order to accommodate their needs, and then develop a plan, which I verify with family that the proposal will work for them and obtain the orders.
I am in contact with both mom and the PHS infusion nurse weekly to obtain information for the nutrition assessment. We discuss Emma’s progress for the week and identify any areas that need to be adjusted, and then I use this information to create recommendations that ultimately get sent to the physician’s office for his review and approval if needed. The open lines of communication between all of the caregivers in the home and clinic ensure that all of Emma’s needs are being met.
Originally published: August 8, 2014

